Coming soon the interactive english version.
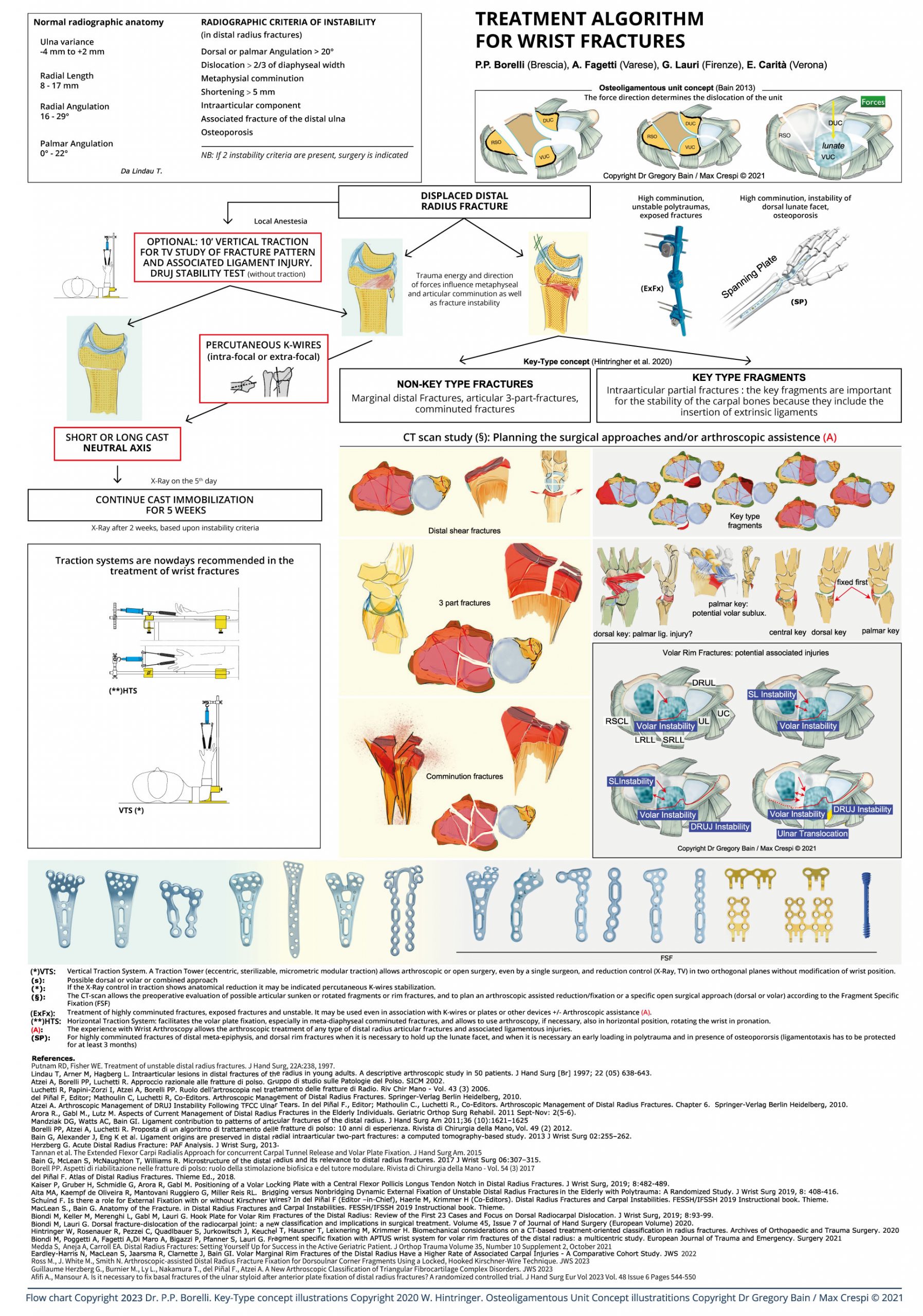
A wrist fracture treatment algorithm, after 10 years of presentations at congresses, was first published in the SICM Hand Surgery Journal in 2012. During the 10 years from 2002 to 2012 angular stability volar plate systems, which slowly evolved from the fixed angle to the polyaxial variable angle, became evident. What has changed in the past 8 years?
The CT scan which increasingly guides, in each classification system, the treatment of a wrist fracture with radiological signs of instability has been enhanced with new technologies such as the “cone beam” CT scan, from maxillofacial applications. CTCB is increasingly replacing traditional CT in anatomical districts such as the wrist and hand, and thanks to lower ionizing radiation emissions with higher and higher resolution, it can often replace traditional radiological scans when a bone impingement or a “gap” or an articular “step-off” or an evolving bone consolidation process must be better interpreted.
MRI with the new high-field machines (1.5 3T) remains the gold standard in the diagnosis of associated ligament injuries.
External fixators have maintained their niche role and have evolved with sterile disposable kits and increased assembly simplicity (only 1 tool to assemble all of the components).
The “spanning plate” (also called bridge plate or distraction plate or Internal Fixator), increasingly used in articular fractures with severe and marginal comminution and in polytrauma patients with bilateral fractures, has joined the rejuvenated External Fixator, and competes with this for offer greater stability with minimal joint distraction (the percentage of the known secondary algodystrophy is reduced) and to eliminate the problem of infection of the fisches especially when the consolidation process takes more than 3 months (osteoporotic bone of the elderly). However the choice is still a dependent surgeon strategy.
It is above all curious to note the return to FSF (Fragment Specific Fixation) which characterized the fixation of wrist fractures in the 90s, that is, increasingly focused on an anatomical stable reduction of single fragments with multiple surgical, volar, dorsal or combined approaches. In recent years surgical sets have gradually developed with plates of various shapes, with hooks incorporated at the distal end, and with “hook plates” increasingly dedicated to the variable sizes of marginal fragments or “key fragments” (fragments with ligament connections) or to those fragments that give stability to the entire assembly and therefore to the wrist as a whole. The market has turned towards a search for a fixation system as complete as possible to manage all the fragments of each size of a complex fracture in a stable way. The challenge is still open even if we have to recognize that some systems, including the one represented in the algorithm, have perhaps completed the “puzzle” of devices capable of addressing all the representation variables of distal radius and ulna fractures.
However, we must not forget the variable of associated ligament injuries which makes it more justified for a surgeon to deepen their experience in wrist arthroscopy. The argument is still controversial. There are in fact expert surgeons who do not consider arthroscopic application necessary for a good anatomical reduction and relative stable fixation of a wrist fracture and who rightly believe that an associated ligament injury may also be suspected by the particular direction of the fracture line on a standard x-ray and diagnosed with dynamic radiological examinations ( “stress view” under traction or dynamic fluoroscopy for the interosseous ligaments of the first row ), or with clinical tests (ballottement test for the TFCC complex ligament), tests performed preoperatively (traction stress view) or, more frequently, once fracture fixation has been performed.
However, it is necessary to recognize the role achieved by wrist arthroscopy in the treatment of wrist fractures, precisely for the evaluation of associated ligament injuries or superficial osteocartilaginous injuries, often not detected from standard x-rays. After suspecting it, it is important to “quantify” (remember the ability of spontaneous healing of most ligament injuries!) and possibly treat an associated ligament injury or highlight and remove a free “osteocartilage” body or partial detachment (site of a subsequent potential osteoarthritis), and/or to adapt the postoperative rehabilitation process to the necessary time required to heal the associated ligament injury, so as to modify what was mistakenly believed, with the advent of angular stability plates, regarding the importance of early mobilization for a good functional result, what seemed to be obtainable thanks to angle stability plates.
Perhaps the most striking aspect over the past 10 years, precisely with the rapid evolution and spread of arthroscopic techniques, has been the tendency to increasingly reduce the need for classic surgical approaches. In practice, a complex fracture can be treated today with combined approaches (volar and dorsal, less invasive) thanks to the shapes of the latest generation plates, or with only volar approaches (“volar plate pre-setting”) and to obtain a reduction, as anatomical as possible, of the articular surface with arthroscopic assistance and then complete a stable fixation with mini-plates or screws, or even with only “headless” screws, through minimally invasive accesses or inserted percutaneously. Are we developing an “beyond the plate” fixation model ?. It would seem that in some situations that screws, if properly applied, can actually replace a plate. (https://chirurgiadellamanobrescia.it/atlas-on-drfs/)
Another aspect to be highlighted is the evolution of Traction Systems that can facilitate wrist fracture treatment throughout its process. From the initial diagnosis and better understanding of the “fracture model” ( under local anesthesia, before performing a temporary or definitive cast) that only a “stress view” with the Traction Tower can immediately reveal, to the reduction options available on the operating table, both in horizontal and in vertical traction, which can undoubtedly facilitate the reduction of complex metadiaphyseal, volar and dorsal fragmentation, or fragmentation of the articular surface, and make arthroscopic applications more and more frequent and justified by the experience that a surgeon acquires following the necessary learning curve.
And the challenge towards a Guideline that can help the surgeon, with the latest concepts on associated extrinsic and ixtrinsic ligament injuries, without closing him in a rigid system but looking like a “recommended” path to follow in order to identify the best strategy for treating a wrist fracture, continues…
References
Putnam MD, Fisher MD. Treatment of unstable distal radius fractures. J Hand Surg, 22A:238,1997.
Lindau T, Arner M, Hagberg L. Intraarticular lesions in distal fractures of the radius in young adults. A descriptive arthroscopic study in 50 patients. J Hand Surg [Br] 1997; 22 (05) 638-643.
Atzei A, Borelli PP, Luchetti R. Approccio razionale alle fratture di polso. Gruppo di studio sulle Patologie del Polso. SICM 2002.
Luchetti R, Papini-Zorzi I, Atzei A, Borelli PP. Ruolo dell’artroscopia nel trattamento delle fratture di Radio. Riv Chir Mano – Vol. 43 (3) 2006.
del Piñal F, Editor; Mathoulin C, Luchetti R, Co-Editors. Arthroscopic Management of Distal Radius Fractures. Springer-Verlag Berlin Heidelberg, 2010.
Atzei A. Arthroscopic Management of DRUJ Instability Following TFCC Ulnar Tears. In del Piñal F., Editor; Mathoulin C., Luchetti R., Co-Editors. Arthroscopic Management of Distal Radius Fractures. Chapter 6. Springer-Verlang Berlin Heidelberg, 2010.
Arora R., Gabl M., Lutz M. Aspects of Current Management of Distal Radius Fractures in the Elderly Individuals. Geriatric Orthop Surg Rehabil. 2011 Sept-Nov: 2(5-6).
Mandziak DG, Watts AC, Bain GI. Ligament contribution to patterns of articular fractures of the distal radius. J Hand Surg Am 2011;36 (10):1621–1625
Borelli PP, Atzei A, Luchetti R. Proposta di un algoritmo di trattamento delle fratture di polso: 10 anni di esperienza. Rivista di Chirurgia della Mano, Vol. 49 (2) 2012.
Bain G, Alexander J, Eng K et al. Ligament origins are preserved in distal radial intraarticular two-part fractures: a computed tomography-based study. 2013 J Wrist Surg 02:255–262.
Herzberg G. Acute Distal Radius Fracture: PAF Analysis. J Wrist Surg, 2013.
Tannan et al. The Extended Flexor Carpi Radialis Approach for concurrent Carpal Tunnel Release and Volar Plate Fixation. J Hand Surg Am. 2015
Bain G, McLean S, McNaughton T, Williams R. Microstructure of the distal radius and its relevance to distal radius fractures. 2017 J Wrist Surg 06:307–315.
Borell PP. Aspetti di riabilitazione nelle fratture di polso: ruolo della stimolazione biofisica e del tutore modulare. Rivista di Chirurgia della Mano – Vol. 54 (3) 2017
del Piñal F. Atlas of Distal Radius Fractures. Thieme Ed., 2018.
Kaiser P, Gruber H, Schmidle G, Arora R, Gabl M. Positioning of a Volar Locking Plate with a Central Flexor Pollicis Longus Tendon Notch in Distal Radius Fractures. J Wrist Surg, 2019; 8:482-489.
Aita MA, Kaempf de Oliveira R, Mantovani Ruggiero G, Miller Reis RL. Bridging versus Nonbridging Dynamic External Fixation of Unstable Distal Radius Fractures in the Elderly with Polytrauma: A Randomized Study. J Wrist Surg 2019, 8: 408-416.
Schuind F. Is there a role for External Fixation with or without Kirschner Wires? In del Piñal F (Editor –in-Chief), Haerle M, Krimmer H (Co-Editors). Distal Radius Fractures and Carpal Instabilities. FESSH/IFSSH 2019 Instructional book. Thieme.
MacLean S., Bain G. Anatomy of the Fracture. in Distal Radius Fractures and Carpal Instabilities. FESSH/IFSSH 2019 Instructional book. Thieme.
Biondi M, Keller M, Merenghi L, Gabl M, Lauri G. Hook Plate for Volar Rim Fractures of the Distal Radius: Review of the First 23 Cases and Focus on Dorsal Radiocarpal Dislocation. J Wrist Surg, 2019; 8:93-99.
Bergsma M, Doornberg JN, Hendrickx L, Hayat B, Kerkhoffs GMMJ, Jhadav B, Jaarsma, RL, Bain G. Interpretations of the Term “Watershed Line” Used as Reference for Volar Plating. J Wrist Surg November 2019
Sun GTW, MacLean SBM, Alexander JJ, Woodman R, Bain G. Association of scapholunate dissociation and two-part articular fractures of the distal radius. Journal of Hand Surgery (European Volume) 0(0) 1–7 2019
Biondi M, Lauri G. Dorsal fracture-dislocation of the radiocarpal joint: a new classification and implications in surgical treatment. Volume 45, Issue 7 of Journal of Hand Surgery (European Volume) 2020.
Hintringer W, Rosenauer R, Pezzei C, Quadlbauer S, Jurkowitsch J, Keuchel T, Hausner T, Leixnering M, Krimmer H. Biomechanical considerations on a CT‐based treatment‐oriented classification in radius fractures. Archives of Orthopaedic and Trauma Surgery. 2020
Biondi M, Poggetti A, Fagetti A,Di Maro A, Bigazzi P, Pfanner S, Lauri G. Fragment specific fixation with APTUS wrist system for volar rim fractures of the distal radius: a multicentric study. European Journal of Trauma and Emergency. Surgery 2021
Medda S, Aneja A, Carroll EA. Distal Radius Fractures: Setting Yourself Up for Success in the Active Geriatric Patient. J Orthop Trauma Volume 35, Number 10 Supplement 2, October 2021
Eardley-Harris N, MacLean S, Jaarsma R, Clarnette J, Bain GI. Volar Marginal Rim Fractures of the Distal Radius Have a Higher Rate of Associated Carpal Injuries – A Comparative Cohort Study. JWS 2021
Chiri W, MacLean SBM, Clarnette J, Eardley-Harris N, White J, Bain G. Anatomical and Clinical Concepts in Distal Radius Volar Ulnar Corner fractures. J Wrist Surg 2022;11:238–249.
Clarnette J, De Silva A, Eardley-Harris N, MacLean S, Bain G. Volar Lunate Facet Fractures of the Distal Radius: Fracture Mapping Using 3D CT Scans. J Wrist Surg 2022
Orbay J, Bain G. Volar Rim Fractures of the Distal Radius: Can We Reduce the Complications and Need for Revision Surgery? J Wrist Surg 2022;11:191–194.
Ross M., J. White M., Smith N. Arthroscopic-assisted Distal Radius Fracture Fixation for Dorsoulnar Corner Fragments Using a Locked, Hooked Kirschner-Wire Technique. JWS 2023
Guillaume Herzberg G., Burnier M., Ly L., Nakamura T., del Piñal F., Atzei A. A New Arthroscopic Classification of Triangular Fibrocartilage Complex Disorders. JWS 2023
Afifi A., Mansour A. Is it necessary to fix basal fractures of the ulnar styloid after anterior plate fixation of distal radius fractures? A randomized controlled trial. J Hand Surg Eur Vol 2023 Vol. 48 Issue 6 Pages 544-550
Crowe CS, Kakar S. Periarticular distal radius fractures and complex ligamentous injury: The role of arthroscopic evaluation. Journal of Orthopaedics 42 (2023) 6–12
Maling L, Smith A. Questions, answers and challenges: Summarising the guidance for distal radius fractures. Journal of Orthopaedics 42 (2023) 47–49
Dhandapani B, Wahegaonkar A. Distal radius fractures-Why do they fail? Journal of Orthopaedics 49 (2024) 24–32
Bhat AK, Fijad NR, Acharya AM. Morphometry of sigmoid notch: A novel method of shape assessment for clinical practice. Journal of Orthopaedics 47 (2024) 80–86
Nordback PH, Ragupathi T, Cheah AEJ. A proposed paradigm shift in the management of distal radius fractures. Journal of Orthopaedics 49 (2024) 117–122
Tuano KR, Mudgal CS. Management of isolated volar lunate facet fractures of the distal radius. Journal of Orthopaedics 51 (2024) 46–53
Ramtin S, Davids F, Farhoud AR, Tejada R, Ring D. The Impact of a Computer-Based Interactive Informed Consent for Surgery on Decision Conflict. Article in press. J Hand Surg Am. 2024
Watch the italian version of the proposal treatment algorithm